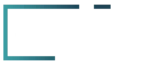A SLAP tear is a shoulder injury affecting the labrum’s upper part. It causes pain and limits motion. This post explains its causes, symptoms, and treatment options to help you understand how to manage and recover from a SLAP tear.
Key Takeaways
- SLAP tears, affecting the superior labrum, can lead to significant shoulder pain and dysfunction, impacting overall stability and function.
- Common causes include acute trauma, repetitive motions in sports, and aging, making early recognition of symptoms essential for effective treatment.
- Treatment options range from non-surgical methods like physical therapy to surgical interventions, with successful outcomes dependent on adherence to rehabilitation protocols.
Understanding SLAP Tears
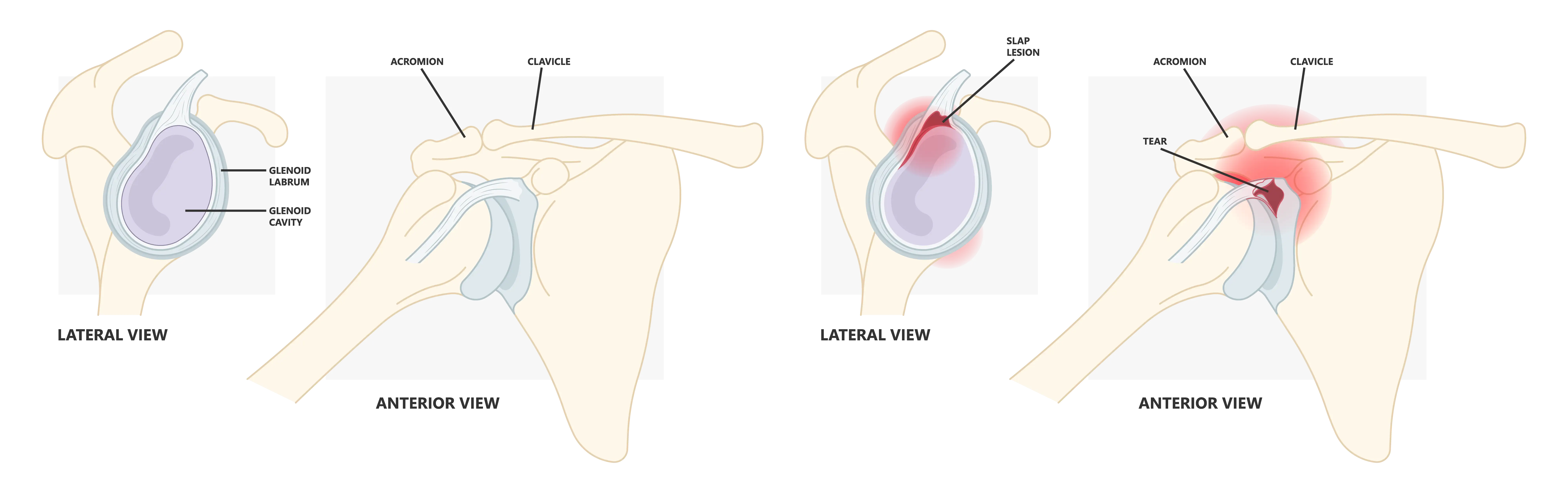
SLAP tears refer to injuries of the superior labrum, a key structure in the shoulder joint. SLAP stands for Superior Labrum Anterior and Posterior, indicating that the injury affects the superior part of the labrum.
A SLAP tear impacts the connection between the bicep tendon and the shoulder blade socket. This can range from minor fraying to a complete detachment of the labrum, causing considerable shoulder pain and dysfunction.
Anatomy of the Shoulder
The shoulder functions as a ball-and-socket joint allowing a wide range of motion. The labrum, a ring of cartilage around the shoulder socket, supports and stabilizes this joint. The tendon of the long head of the biceps muscle attaches to the labrum, essential for shoulder movement and stability.
Labrum injuries can destabilize the shoulder joint, causing chronic pain and limited range of motion. Knowledge of shoulder anatomy highlights the significant impact SLAP tears and shoulder labral tear can have on daily activities and athletic performance.
Causes of SLAP Tears
SLAP tears can be attributed to several causes, with acute trauma, repetitive shoulder motion, and aging being the most common. Acute injuries often result from falls or heavy lifting, accounting for a significant percentage of shoulder injuries. Sports that involve repetitive overhead motions, like baseball or tennis, put athletes at higher risk.
Laborers in physically demanding jobs, such as weightlifters or factory workers, also face a risk of SLAP tears due to the repetitive strain on their shoulders. Aging can further exacerbate the risk as the labrum deteriorates over time, making it more susceptible to tears. Recognizing these causes is key for prevention and early intervention, especially in high-risk groups.
Recognizing Symptoms of SLAP Tears
Symptoms of SLAP tears vary but often include shoulder pain, limited range of motion, and weakness. These symptoms can interfere with daily activities and sports performance, making early recognition essential for effective treatment.
Some individuals with SLAP tears may experience a sensation of instability, catching, or clicking in the shoulder, although symptoms can vary widely. In addition to pain, individuals may notice a decrease in their ability to use the affected arm, impacting both strength and function.
Another common symptom is a clicking or popping sensation during shoulder movements, which can be quite disconcerting. Early recognition of these symptoms can lead to quicker diagnosis and more effective treatment options.
Diagnosing SLAP Tears
Diagnosing SLAP tears requires a comprehensive approach, beginning with a detailed medical history and physical examination. Specialized tests, such as the biceps load test and active compression test, assess shoulder function and identify potential SLAP tears.
Imaging techniques are important for diagnosis. Typically, an MRI visualizes soft tissues like the labrum, while an MR arthrogram, involving dye injection into the joint, provides more detailed images. X-rays may also be ordered to rule out issues like arthritis or fractures.
Diagnosing SLAP tears can be challenging due to their tendency to occur alongside other shoulder injuries. A qualified shoulder specialist can evaluate shoulder symptoms and determine whether further testing or treatment may be appropriate.
Treatment Options for SLAP Tears
Treatment options for SLAP tears vary from non-surgical to slap tear surgery interventions, depending on the tear’s severity and the patient’s specific needs.
These options can be explored in detail to determine the best course of action for managing SLAP tears.
Non-Surgical Treatments
Initially, SLAP injuries are typically managed with non-surgical options. Rest and physical therapy are often recommended to alleviate symptoms and restore shoulder function. Physical therapy strengthens the shoulder muscles and improves joint control. Medications like nonsteroidal anti-inflammatory drugs (NSAIDs) may be recommended to reduce inflammation and pain.
Surgical Treatments
Severe SLAP tears may require surgical intervention. Arthroscopic surgery, a minimally invasive technique, repairs the labrum with small incisions, minimizing damage to surrounding tissues. One common method is the SLAP repair, suturing the labrum to the shoulder socket bone.
In some cases, particularly in older patients or those with biceps tendon involvement, biceps tenodesis may be recommended instead of a traditional SLAP repair. In this procedure, the biceps tendon is detached from its attachment on the labrum and reattached to the upper arm bone (humerus). This approach can relieve pain and improve function, especially when the biceps tendon is contributing to symptoms.
Post-Surgery Rehabilitation
Post-surgery rehabilitation plays an important role in restoring shoulder function. A sling is typically used for four to six weeks to support the shoulder and facilitate healing. Physical therapy begins shortly after surgery to restore strength, endurance, and pain-free range of motion.
Return to sports after SLAP repair varies. Many athletes take approximately 4 to 6 months or longerbefore returning to higher-level activities, depending on healing and rehabilitation progress. A well-structured program is essential for successful recovery.
Recovery Times
Recovery times vary based on surgery complexity and individual factors. Complete recovery for recreational activities or sports might take six to twelve months. Adherence to rehabilitation protocols is important for the success of the surgery and overall recovery.
Many patients report improvement in pain and shoulder function following SLAP repair, though outcomes can vary depending on factors such as age, activity level, and the presence of other shoulder conditions. Recovery can span from several months to over a year.
Potential Complications if Untreated
Ignoring a SLAP tear can lead to chronic pain and persistent shoulder instability. In some cases, ongoing shoulder dysfunction from an untreated SLAP tear may contribute to continued shoulder pain or additional stress on surrounding structures.
Neglecting a SLAP tear can result in compensatory injuries in other parts of the shoulder or arm, exacerbating the problem and complicating treatment. Early intervention is important for preventing these complications and ensuring a better quality of life.
Related Shoulder Injuries
SLAP tears are often associated with other shoulder injuries, especially in sports-related contexts where repetitive overhead activities are common. These activities significantly increase the risk of developing SLAP tears and related injuries.
Common related injuries include biceps tendonitis, rotator cuff injuries, and other labral tears. Recognizing the interconnected nature of these injuries is key for comprehensive shoulder care and effective treatment.
Summary
In summary, SLAP tears can significantly impact daily life and athletic performance, but understanding their causes, symptoms, and treatment options can lead to effective management and recovery. Both non-surgical and surgical treatments are available, each with its own benefits and considerations. If you suspect a SLAP tear, early diagnosis and treatment are important steps to prevent additional complications, and they can support a more successful recovery.
Frequently Asked Questions
What is a SLAP tear?
A SLAP tear is an injury to the superior portion of the labrum, the ring of cartilage surrounding the shoulder socket, where the long head of the biceps tendon attaches. This injury can cause pain and instability in the shoulder, often requiring medical attention.
What are the common symptoms of a SLAP tear?
Common symptoms of a SLAP tear include shoulder pain, instability, reduced range of motion, and clicking or popping sensations during movement. If you experience these, it’s important to consult a doctor for an evaluation.
How is a SLAP tear diagnosed?
A SLAP tear is diagnosed through a combination of medical history, physical examination, specialized tests, and imaging techniques such as MRI or MR arthrogram. This comprehensive approach supports an accurate assessment and diagnosis.
What are the treatment options for SLAP tears?
The treatment options for SLAP tears comprise non-surgical methods like rest, physical therapy, and medications, alongside surgical interventions such as arthroscopic repair and biceps tenodesis. Each approach should be tailored to the severity of the injury and individual patient needs.
What is the recovery time for SLAP tear surgery?
The recovery time for SLAP tear surgery typically ranges from six months to a year, with successful outcomes heavily dependent on following rehabilitation protocols.