Shoulder arthritis can make even simple movements, such as brushing your hair, reaching for a shelf, or getting dressed, feel painful and frustrating. A wide range of treatments may help reduce discomfort and support better shoulder function. This post explores various ways to ease arthritis pain in the shoulder, so you can feel more confident navigating your care.
Key Takeaways
- Many patients find relief from shoulder arthritis through non-surgical methods, including physical therapy, activity modification, and anti-inflammatory medications.
- When non-surgical treatments no longer provide adequate relief, advanced surgical options, such as shoulder replacement, may become a recommended option.
- A board-certified orthopedic surgeon specializing in the upper extremity can evaluate your condition and tailor a treatment plan to your needs and lifestyle.
Understanding the Arthritic Shoulder
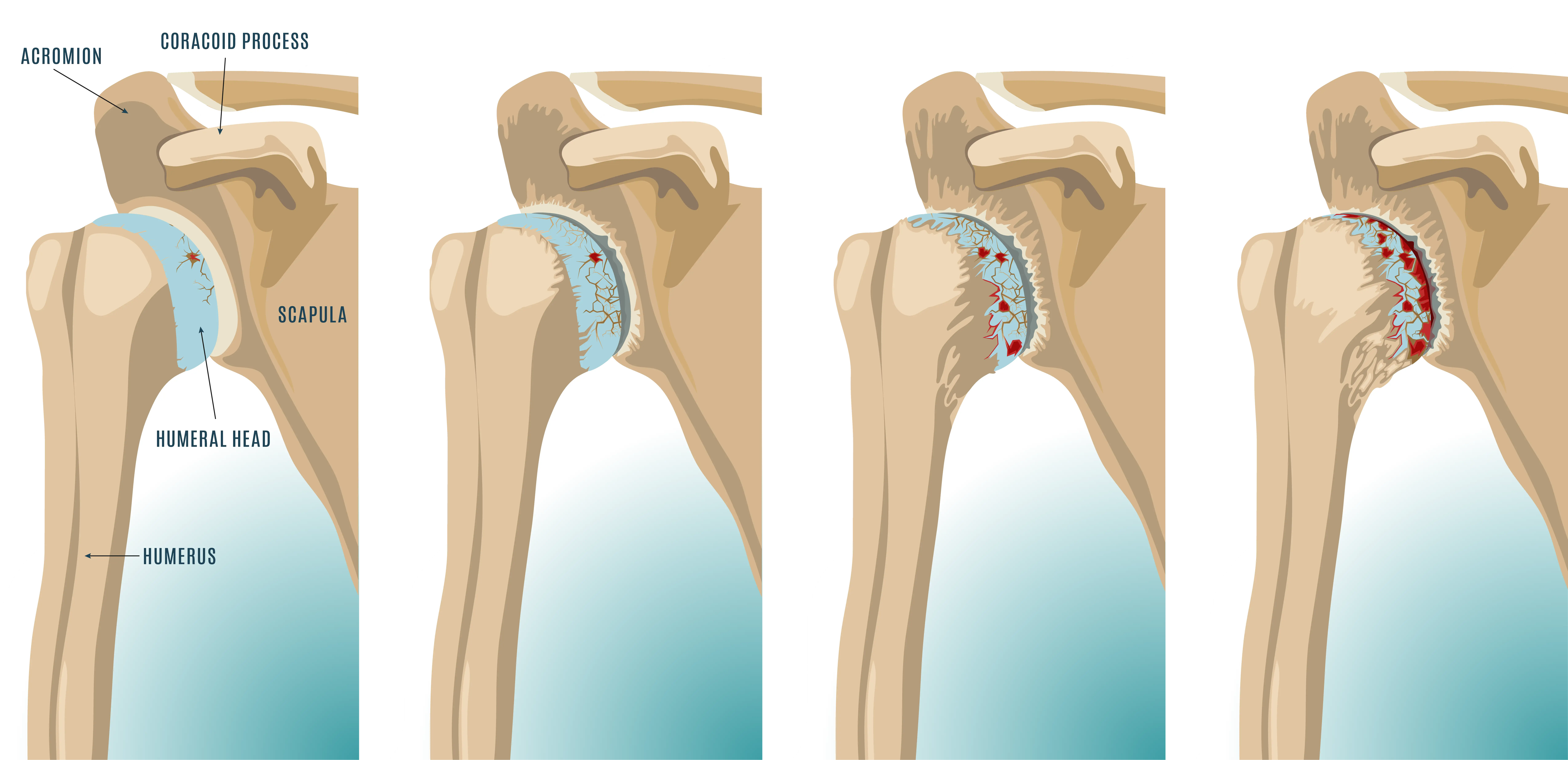
The shoulder is one of the most mobile joints in the body, allowing for an incredible range of motion. This mobility, however, comes at a cost, making it susceptible to wear and tear over time. Arthritis in the shoulder typically affects one or both of the two main joints: the glenohumeral joint (the main ball-and-socket joint) and the acromioclavicular (AC) joint (where the collarbone meets the shoulder blade).
The Types of Shoulder Arthritis
While many conditions can cause joint pain, three primary forms of arthritis commonly affect the shoulder:
- Osteoarthritis (OA): This is the most common type, often called “wear-and-tear” arthritis. It occurs when the smooth cartilage covering the ends of the bones gradually breaks down. As the cartilage wears away, the bones rub against each other, which may cause pain, stiffness, and the formation of bone spurs (osteophytes).
- Rheumatoid Arthritis (RA): RA is an autoimmune disease. This means the body’s immune system mistakenly attacks the lining of the joint capsule, known as the synovium. This attack causes inflammation, swelling, and pain, which can eventually destroy the cartilage and bone. RA can affect both shoulders simultaneously.
- Post-traumatic Arthritis: This form of OA develops after a shoulder injury, such as a fracture or dislocation. The trauma to the joint can damage the cartilage, leading to arthritis years later.
Recognizing the Symptoms
The symptoms of shoulder arthritis often progress gradually. Common symptoms include:
- Pain: It may start as a dull ache and can worsen with activity. As the condition progresses, the pain may become constant, even at rest, and can frequently disrupt sleep.
- Stiffness and Limited Motion: Patients frequently notice a gradual loss of the ability to move the arm. Reaching overhead, behind the back, or across the body becomes increasingly difficult.
- Grinding, Clicking, or Catching: As the cartilage disappears, the rough surfaces of the bones may rub together, producing a grinding sensation or sound, known as crepitus.
- Tenderness: The joint may feel tender to the touch.
Non-Surgical Strategies
For many patients, the initial treatment plan focuses on conservative, non-surgical methods. These strategies aim to reduce inflammation, manage pain, and preserve joint function.
Activity Modification and Rest
Avoiding activities that involve repetitive overhead movements or heavy lifting is often the first step. This usually does not mean you should stop moving entirely. Instead, you should learn to modify your movements to keep the joint within a comfortable range. For example, you might use a reacher tool instead of straining to grab an item from a high shelf.
Physical Therapy and Targeted Exercise
A physical therapist can design a personalized program that focuses on gentle stretching and strengthening. The goal is not to force the joint into painful positions but to maintain the existing range of motion and strengthen the surrounding muscles. Strong muscles may help stabilize the joint and reduce the stress placed directly on the damaged cartilage.
Medications for Pain and Inflammation
Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen and naproxen work by reducing both pain and inflammation. You should always use these medications as directed by your doctor. Acetaminophen primarily targets pain and does not reduce inflammation. It may be an option for patients who cannot tolerate NSAIDs.
Thermal Therapy: Heat and Ice
Alternating between heat and cold may provide simple relief at home.
- Ice: Applying a cold pack for 15 to 20 minutes several times a day can help reduce swelling and numb the pain, particularly after activity or during a flare-up.
- Heat: Moist heat, such as a warm shower or a heating pad, can relax stiff muscles and increase blood flow to the area.
Surgical Solutions
Despite the best efforts with non-surgical treatments, shoulder arthritis can sometimes progress to a point where the pain is constant and severely limits function. When this happens, surgery may become the recommended option, with the goal of providing long-term pain relief and functional restoration.
Arthroscopy
In the early stages of arthritis, or for specific types like AC joint arthritis, a minimally invasive procedure called arthroscopy may be an option. The surgeon uses a small camera and instruments to clean out the joint. This might involve removing loose fragments of cartilage or bone spurs (debridement) that are causing mechanical symptoms like catching or locking. While arthroscopy can provide temporary relief, it does not generally stop the progression of the underlying arthritis.
Shoulder Replacement (Arthroplasty)
Shoulder replacement surgery is a treatment for advanced arthritis. This procedure involves replacing the damaged parts of the shoulder joint with artificial components (implants). The two primary types of shoulder replacement are:
- Total Shoulder Arthroplasty: This procedure replaces both the ball (head of the humerus) and the socket (glenoid) with prosthetic components. It is typically used when the rotator cuff tendons are healthy and intact.
- Reverse Total Shoulder Arthroplasty: In this procedure, the ball and socket are reversed. The ball is placed on the shoulder blade side, and the socket is placed on the arm bone side. This design allows the patient to use the deltoid muscle instead of the damaged rotator cuff to lift the arm. Reverse shoulder replacement is often the preferred choice for patients with severe arthritis who also have a large, irreparable rotator cuff tear (rotator cuff tear arthropathy).
Post-operative rehabilitation is an important part of the recovery process, supporting the best possible long-term outcome.
Summary
Living with shoulder arthritis presents significant challenges, but there are many options available to manage your symptoms and improve your quality of life. Learning how to ease arthritis pain in the shoulder is a process that requires patience, consistency, and a partnership with a trusted orthopedic specialist. Many patients find meaningful relief through a combination of non-surgical treatments. When these conservative measures are no longer effective, modern surgical techniques, particularly shoulder replacement, may be recommended.
Frequently Asked Questions
Can I still exercise if I have shoulder arthritis?
Generally, yes. Low-impact exercise is typically recommended. You should focus on gentle range-of-motion exercises and strengthening the surrounding muscles. Avoid high-impact or heavy lifting activities that cause sharp pain.
What is the difference between AC joint arthritis and glenohumeral arthritis?
Glenohumeral arthritis affects the main ball-and-socket joint. AC joint arthritis affects the smaller joint at the top of the shoulder (where the collarbone meets the shoulder blade), often causing localized pain when reaching across the body or sleeping on the affected side.
When should I see an orthopedic surgeon instead of my primary care doctor?
Consider consulting an orthopedic surgeon specializing in the shoulder if your pain is persistent, significantly limits your daily activities, or if conservative treatments have failed to provide adequate relief after several weeks. An orthopedic specialist may be able to offer a wider range of advanced treatment options.