Shoulder pain can significantly impact daily life, limiting movement and causing discomfort. Often, this pain stems from arthritis, a condition characterized by inflammation and degeneration of the joint. In this post, we’ll take a closer look at shoulder arthritis, exploring its various causes and outlining effective treatment options.
Key Takeaways
- Arthritis in the shoulder involves the breakdown of cartilage in the joint, leading to pain, stiffness, and reduced mobility.
- The condition can arise from various factors, including age-related wear and tear (osteoarthritis), autoimmune disorders (rheumatoid arthritis), previous injuries (post-traumatic arthritis), severe rotator cuff tears (rotator cuff tear arthropathy), and impaired blood supply to the bone (avascular necrosis).
- Treatment ranges from conservative approaches like activity modification, physical therapy, and medication to surgical interventions, depending on the severity and type of arthritis.
What is Shoulder Arthritis?
Arthritis is a condition characterized by inflammation of one or more joints. In the context of the shoulder, arthritis refers to the deterioration of the smooth cartilage that covers the ends of the bones within the shoulder joint. This cartilage acts as a cushion, allowing the bones to glide smoothly against each other during movement. When this cartilage wears away, bones can rub directly against each other, leading to pain, stiffness, and a reduced range of motion.
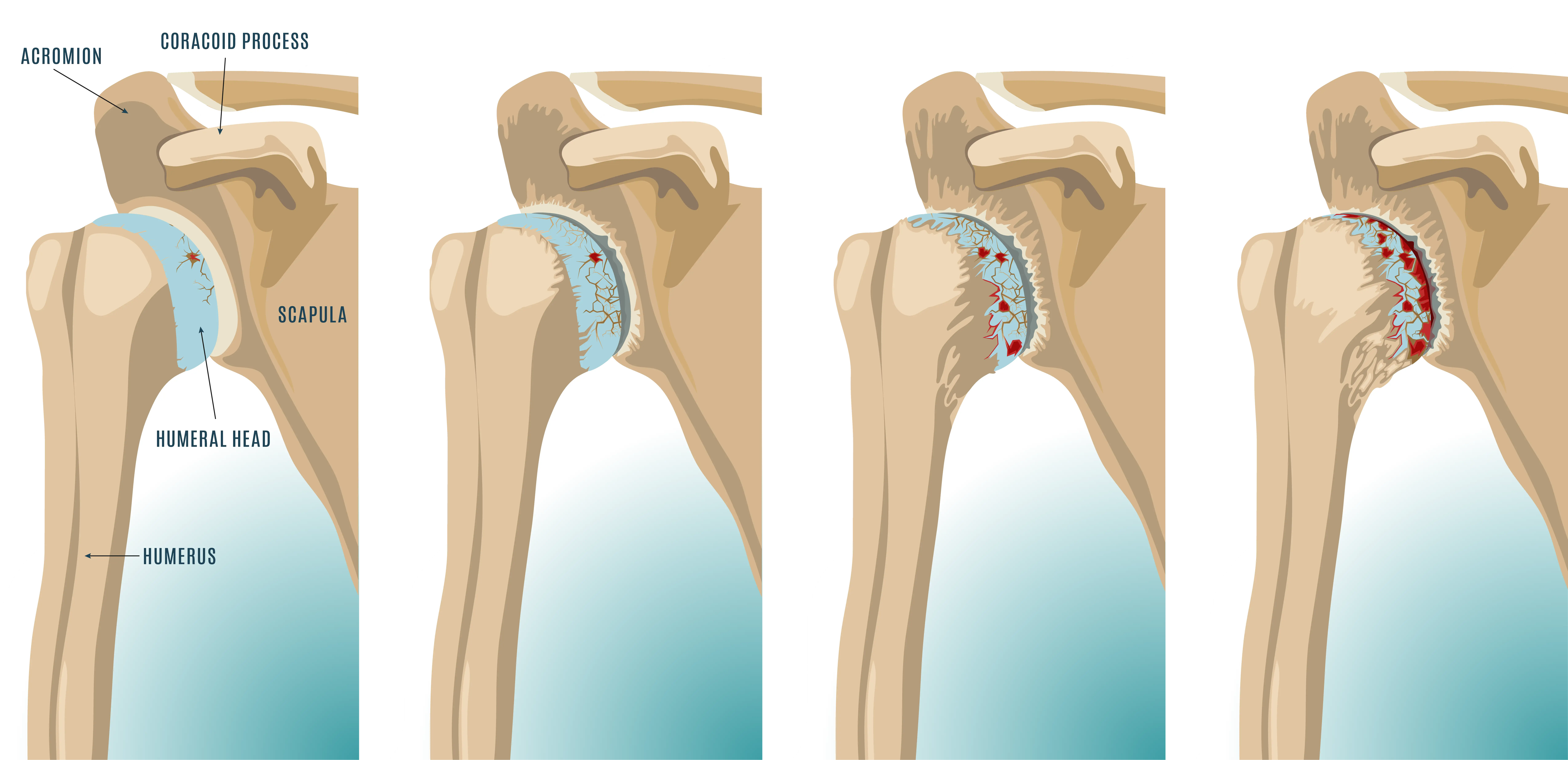
The shoulder is a complex joint, primarily composed of the glenohumeral joint and the acromioclavicular (AC) joint. The glenohumeral joint is the main ball-and-socket joint where the head of the upper arm bone (humerus) fits into the shallow socket of the shoulder blade (glenoid). The AC jointis located at the top of the shoulder, where the collarbone (clavicle) meets the highest part of the shoulder blade (acromion). Both of these joints can be affected by arthritis, though glenohumeral arthritis is more commonly associated with significant pain and functional limitation.
Causes and Types of Shoulder Arthritis
Shoulder arthritis is not a single condition but rather a group of diseases that can affect the shoulder joint. The underlying causes vary depending on the type of arthritis.
Osteoarthritis (OA)
Osteoarthritis, often referred to as “wear-and-tear” arthritis, is the most common form of arthritis affecting the shoulder. It typically develops gradually with age as the cartilage that cushions the ends of the bones wears away. While primary OA has no specific identifiable cause, it is often linked to age and genetics. Secondary OA can result from previous shoulder injuries or conditions that alter the joint mechanics.
Rheumatoid Arthritis (RA)
Rheumatoid arthritisis a chronic autoimmune disease where the body’s immune system mistakenly attacks its own healthy tissues, including the lining of the joints (synovium). This leads to inflammation, pain, swelling, and eventually, joint damage and deformity. RA typically affects multiple joints symmetrically, and the shoulder is a common site of involvement.
Post-Traumatic Arthritis
Post-traumatic arthritis develops after an injury to the shoulder joint. This type of arthritis can occur years after the initial trauma, as the injury disrupts the normal joint mechanics and accelerates cartilage wear.
Rotator Cuff Tear Arthropathy
Rotator cuff tear arthropathy is a severe form of shoulder arthritis that develops in conjunction with a large, long-standing rotator cuff tear. The rotator cuff muscles and tendons are important for stabilizing the shoulder joint and enabling a wide range of motion. When these tendons are severely torn, the humeral head can migrate upwards, leading to abnormal contact and friction between the bones, accelerating cartilage wear.
Avascular Necrosis (AVN)
Avascular necrosis (AVN), also known as osteonecrosis, can occur when the blood supply to the head of the humerus (the ball part of the shoulder joint) is interrupted. Without adequate blood flow, the bone tissue dies and collapses, leading to damage of the overlying cartilage and subsequent arthritis.
Symptoms of Shoulder Arthritis
The symptoms of shoulder arthritis can vary in severity and presentation, but they generally progress over time. Recognizing these signs early can facilitate timely diagnosis and intervention.
Common symptoms include:
- Pain: This is the most prevalent symptom. Initially, pain may only occur during activity or with specific movements. As the arthritis progresses, pain can become constant, even at rest, and may disturb sleep. The pain is frequently described as a deep ache within the joint or radiating to the side of the shoulder.
- Stiffness and Loss of Range of Motion: The shoulder joint may feel stiff, especially after periods of inactivity. Patients often experience a gradual decrease in their ability to move the arm through its full range of motion, making everyday tasks like reaching overhead, dressing, or washing hair challenging.
- Grinding, Clicking, or Popping Sensations (Crepitus): As the cartilage wears away and bone surfaces rub against each other, patients may hear or feel grinding, clicking, or popping noises within the joint. These sensations may or may not be accompanied by pain.
- Weakness: Due to pain and reduced mobility, the muscles surrounding the shoulder may weaken, further impacting function.
- Tenderness: The joint may be tender to the touch, particularly along the joint line.
Diagnosis of Shoulder Arthritis
Accurate diagnosis of shoulder arthritis involves a comprehensive approach, combining a thorough medical history, physical examination, and imaging studies. Your doctor will likely inquire about symptoms, their duration, severity, and any history of shoulder injuries or medical conditions.
The physical exam may involve assessing the shoulder’s range of motion (both active and passive), strength, stability, and identifying areas of tenderness. Your doctor may perform specific tests to differentiate between various shoulder conditions.
Imaging tests may be needed to confirm the diagnosis. Standard X-rays are often the first imaging modality used. They can reveal narrowing of the joint space (indicating cartilage loss), bone spurs, and changes in bone structure. Magnetic resonance imaging (MRI) provides detailed images of soft tissues, including cartilage, tendons (like the rotator cuff), and ligaments. It can help assess the condition of the rotator cuff and identify other soft tissue pathologies that may be contributing to symptoms.
Treatment Options for Shoulder Arthritis
The treatment for shoulder arthritis is tailored to the individual patient, considering the type and severity of arthritis, the patient’s age, activity level, and overall health. Treatment typically begins with conservative, non-surgical approaches. If these are unsuccessful or the arthritis is severe, surgical options may be considered.
Conservative (Non-Surgical) Treatments
These methods aim to reduce pain, improve function, and slow the progression of arthritis without surgery.
- Activity Modification: Avoiding or reducing activities that aggravate shoulder pain is often the first step. This might involve modifying sports activities, lifting techniques, or occupational tasks.
- Ice and Heat: Applying ice packs to the affected shoulder can help reduce inflammation and pain, especially after activity. Moist heat can help relax muscles and improve stiffness. Patients may find one more effective than the other, or a combination of both.
- Physical Therapy and Exercise: A structured physical therapy program is often important for maintaining or improving shoulder mobility, strength, and flexibility. Exercises focus on gentle range-of-motion, stretching, and strengthening the muscles around the shoulder to provide better support and stability. A physical therapist can design an individualized program.
- Nonsteroidal Anti-inflammatory Drugs: NSAIDs can help manage pain and reduce inflammation.
- Corticosteroid Injections: Injections directly into the shoulder joint can provide significant, albeit temporary, relief from pain and inflammation.
- PRP Injections: Platelet-rich plasma injections may help promote healing in the area.
Surgical Treatments
When conservative treatments fail to provide adequate relief, or if the arthritis is advanced and impacting quality of life, surgical intervention may be recommended. The choice of surgical procedure depends on the type and severity of arthritis, the patient’s age, activity level, and the condition of the surrounding soft tissues, particularly the rotator cuff. An experienced shoulder surgeon can evaluate the condition and help guide the most appropriate treatment path.
Arthroscopic debridement is a minimally invasive procedure that involves inserting a small camera (arthroscope) and instruments through small incisions to clean out the joint. The surgeon can remove loose fragments of cartilage, bone spurs, and inflamed tissue. This procedure is typically reserved for early-stage arthritis or when symptoms are primarily mechanical (e.g., catching or locking).
Total shoulder replacement involves replacing both the humeral head and the glenoid socket with prosthetic components. The humeral head is replaced with a metal ball attached to a stem inserted into the humerus, and the glenoid is resurfaced with a smooth plastic component. For many patients, this procedure can be highly effective in relieving pain and restoring function in patients with severe glenohumeral osteoarthritis and an intact rotator cuff.
Reverse shoulder replacement is a specialized type of shoulder replacement primarily designed for patients with severe arthritis accompanied by a massive, irreparable rotator cuff tear (rotator cuff tear arthropathy). In a reverse total shoulder replacement, the ball and socket components are switched: a metal ball is fixed to the shoulder blade, and a plastic socket is attached to the upper arm bone. This design allows the deltoid muscle to power the arm, compensating for the non-functional rotator cuff.
Prevention of Shoulder Arthritis
While not all forms of shoulder arthritis are entirely preventable, there are several strategies that can help reduce the risk of developing certain types of arthritis and manage symptoms.
- Regular, Low-Impact Exercise: Engaging in regular physical activity that strengthens the muscles around the shoulder and maintains joint flexibility supports joint function. Low-impact exercises, such as swimming, cycling, or specific shoulder exercises prescribed by a physical therapist, can help without putting excessive stress on the joint.
- Protect Your Shoulders from Injury: Taking precautions to prevent shoulder injuries, such as using proper lifting techniques, wearing protective gear during sports, and avoiding falls, can reduce the risk of post-traumatic arthritis.
- Early Detection and Management: If you experience persistent shoulder pain or stiffness, seeking medical attention early is important. Early diagnosis allows for timely intervention and the implementation of conservative strategies that can help manage symptoms.
Summary
Shoulder arthritis is a condition that can significantly impair an individual’s quality of life, causing persistent pain, stiffness, and loss of function. It encompasses various types, each with distinct causes. Early diagnosis and a tailored treatment plan support effective management. Treatment options span from conservative measures, including activity modification, physical therapy, and various medications, to advanced surgical interventions such as arthroscopic debridement, total shoulder replacement, or reverse total shoulder arthroplasty. The choice of treatment is highly individualized, depending on the specific type and severity of arthritis, as well as patient-specific factors.
Frequently Asked Questions
What is the difference between osteoarthritis and rheumatoid arthritis in the shoulder?
Osteoarthritis is a degenerative condition caused by the wear and tear of cartilage over time, often age-related. Rheumatoid arthritis, on the other hand, is an autoimmune disease where the body’s immune system attacks the joint lining, leading to inflammation and damage. OA typically affects one or a few joints, while RA may affect multiple joints symmetrically.
How long does recovery take after shoulder replacement surgery?
Recovery time varies depending on the type of shoulder replacement (total vs. reverse), individual patient factors, and adherence to rehabilitation protocols. Generally, it can take several months to a year to achieve maximum recovery, with improvement often seen within the first few months. Physical therapy is a key component of the recovery process.
What’s the difference between total and reverse shoulder replacement?
Total shoulder replacement replicates the natural anatomy of the shoulder and may rely on an intact rotator cuff; reverse replacement switches ball-and-socket positions so the deltoid powers the arm, making it a valuable treatment option when the cuff is irreparable.
When should I consider surgery for shoulder arthritis?
If months of non-operative care no longer control pain or function, or if the arthritis is severe, consider discussing your surgical options with a shoulder specialist.