The shoulder is one of the most mobile joints in the human body. It allows us to perform a vast range of movements, from reaching for a high shelf to throwing a ball. When this mobility is compromised, the impact on daily life can be profound. A condition called frozen shoulder, or adhesive capsulitis, is characterized by a significant loss of both active and passive range of motion. Patients often ask, “What causes a frozen shoulder?” In this post, we’ll explore the underlying mechanisms and risk factors.
Key Takeaways
- Frozen shoulder, or adhesive capsulitis, involves the thickening and tightening of the shoulder joint capsule, which is the protective sac surrounding the joint.
- The condition is categorized as primary (idiopathic, meaning the cause is unknown) or secondary (linked to a specific injury, surgery, or underlying health condition).
- A period of prolonged shoulder immobilization, such as after a fracture or surgery, can trigger the condition.
- Frozen shoulder progresses through three distinct phases: freezing, frozen, and thawing.
The Anatomy of Stiffness: How the Shoulder Freezes
To understand what causes a frozen shoulder, we must first look at the shoulder’s structure. Your shoulder is a ball-and-socket joint, where the head of the upper arm bone (humerus) fits into a shallow socket (glenoid) of the shoulder blade. A strong, flexible envelope of connective tissue, called the joint capsule, surrounds this joint. This capsule contains synovial fluid, which lubricates the joint and helps it move smoothly.
In a frozen shoulder, the joint capsule becomes inflamed. This inflammation causes the capsule to thicken, contract, and tighten around the joint. Thick bands of scar tissue, known as adhesions, begin to form within the folds of the capsule. These adhesions can restrict movement. The reduction in synovial fluid also contributes to stiffness.
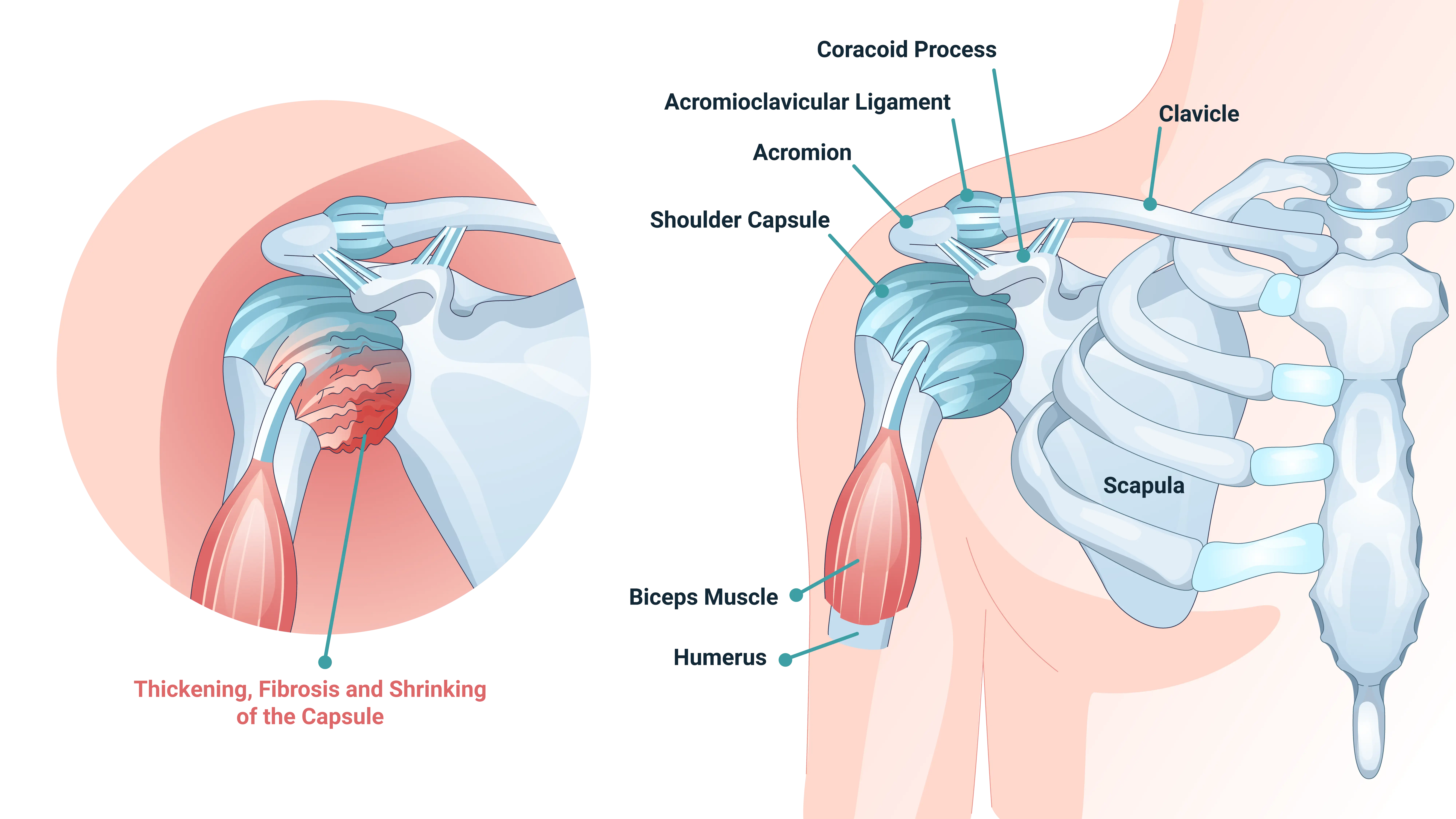
The Central Question: What Causes a Frozen Shoulder?
Frozen shoulder is generally divided into two main types based on the origin of the problem: idiopathic (primary) or secondary.
Primary (Idiopathic) Frozen Shoulder
In many cases, a frozen shoulder develops without any clear preceding event or injury. This is known as primary or idiopathic adhesive capsulitis. The term “idiopathic” simply means the cause is unknown. Causes are still being researched, but some studies suggest that the process may involve an autoimmune or inflammatory response that is triggered.
Secondary Frozen Shoulder
Secondary frozen shoulder occurs when a specific event or underlying medical condition clearly precedes the onset of stiffness. In these cases, the cause is identifiable. The underlying condition acts as a catalyst, setting the stage for the joint capsule to thicken and contract.
Systemic Health Conditions: Risk Factors
While the exact trigger for primary frozen shoulder is elusive, certain systemic health conditions may increase a person’s risk of developing the condition.
- Diabetes Mellitus: Considered one of the strongest risk factors; elevated blood sugar may contribute to changes in the joint capsule and surrounding tissues, making the shoulder more prone to stiffness and adhesions.
- Thyroid Disease: Both overactive and underactive thyroid function are associated with higher rates of frozen shoulder.
- Cardiovascular Disease: Some research suggests that individuals with heart disease, including those with a history of myocardial infection, may have a higher incidence.
- Stroke: Reduced arm movement and potential nerve involvement after a stroke may lead to secondary frozen shoulder.
- Parkinson’s Disease: Decreased arm mobility and muscle rigidity may increase the likelihood of developing shoulder stiffness.
- Autoimmune Conditions: Some autoimmune disorders may contribute to a generalized inflammatory state that can predispose individuals to frozen shoulder.
The Role of Injury, Surgery, and Immobilization
For many patients, the answer to what causes a frozen shoulder lies in a recent event that forced them to keep their arm still. This is a common pathway to secondary frozen shoulder.
Trauma and Injury
A significant injury to the shoulder, even if it does not directly damage the joint capsule, can be the starting point. The key factor here is not the injury itself, but the subsequent lack of movement. When the arm is immobilized for an extended period, the joint capsule’s folds may stick together, and the process of thickening and contraction can accelerate.
Post-Surgical Complications
The post-operative recovery from shoulder surgery often requires a period of immobilization to allow tissues to heal. This rest period carries a risk of developing a frozen shoulder. Surgeons and physical therapists work diligently to balance the need for healing with the need for early, controlled motion to help prevent this complication.
The Three Phases of Frozen Shoulder
Understanding the clinical course of adhesive capsulitis helps patients manage their expectations and recognize the progression of the disease. Frozen shoulder typically evolves through three distinct, overlapping stages.
1. The Freezing Stage (Painful Stage)
This initial phase is marked by the gradual onset of pain. The pain is often dull and aching, but it can worsen at night and with movement. As the pain increases, the range of motion in the shoulder slowly begins to decrease. Patients often try to avoid moving the arm to reduce the pain, which may contribute to the stiffness.
2. The Frozen Stage (Stiff Stage)
During the frozen stage, the pain may actually begin to subside. However, the stiffness becomes much more pronounced. The shoulder’s range of motion is severely limited, making simple tasks like dressing, reaching into a back pocket, or driving very difficult. Although the pain is less intense than in the freezing stage, the functional limitation is frequently at its peak.
3. The Thawing Stage (Recovery Stage)
The thawing stage is the period of recovery. The shoulder’s range of motion slowly and gradually begins to improve. The return of motion can be slow.
Summary
The question of what causes a frozen shoulderdoes not have a single, simple answer. It is a complex condition that arises from a change in the joint capsule, often triggered by a combination of systemic health issues and periods of immobilization. For many, the cause is idiopathic, but for a large number of patients, the condition is a secondary complication.
Understanding these causes and risk factors is the first step toward effective management. Consulting with an orthopedic specialist, particularly one with expertise in the upper extremity, can help you better understand your condition and explore available treatment options.
Frequently Asked Questions
Is a frozen shoulder the same as arthritis?
No, they are different conditions. Shoulder arthritis involves the wear and tear of the joint cartilage, which causes pain and stiffness. A frozen shoulder, or adhesive capsulitis, is a problem with the joint capsule, which thickens and tightens. While both can cause stiffness, the underlying pathology is distinct.
What is the difference between primary and secondary frozen shoulder?
Primary (idiopathic) frozen shoulder has no known cause. Secondary frozen shoulder is caused by an identifiable factor, such as a period of immobilization after an injury, surgery, or a pre-existing systemic condition.
Should I stop moving my arm if it hurts?
While patients should generally avoid movements that cause sharp, intense pain, completely stopping movement can be counterproductive and may worsen a frozen shoulder. Controlled, gentle range-of-motion exercises, often guided by a physical therapist, may help prevent the joint capsule from tightening further. Always consult with your orthopedic specialist before starting any exercise program.